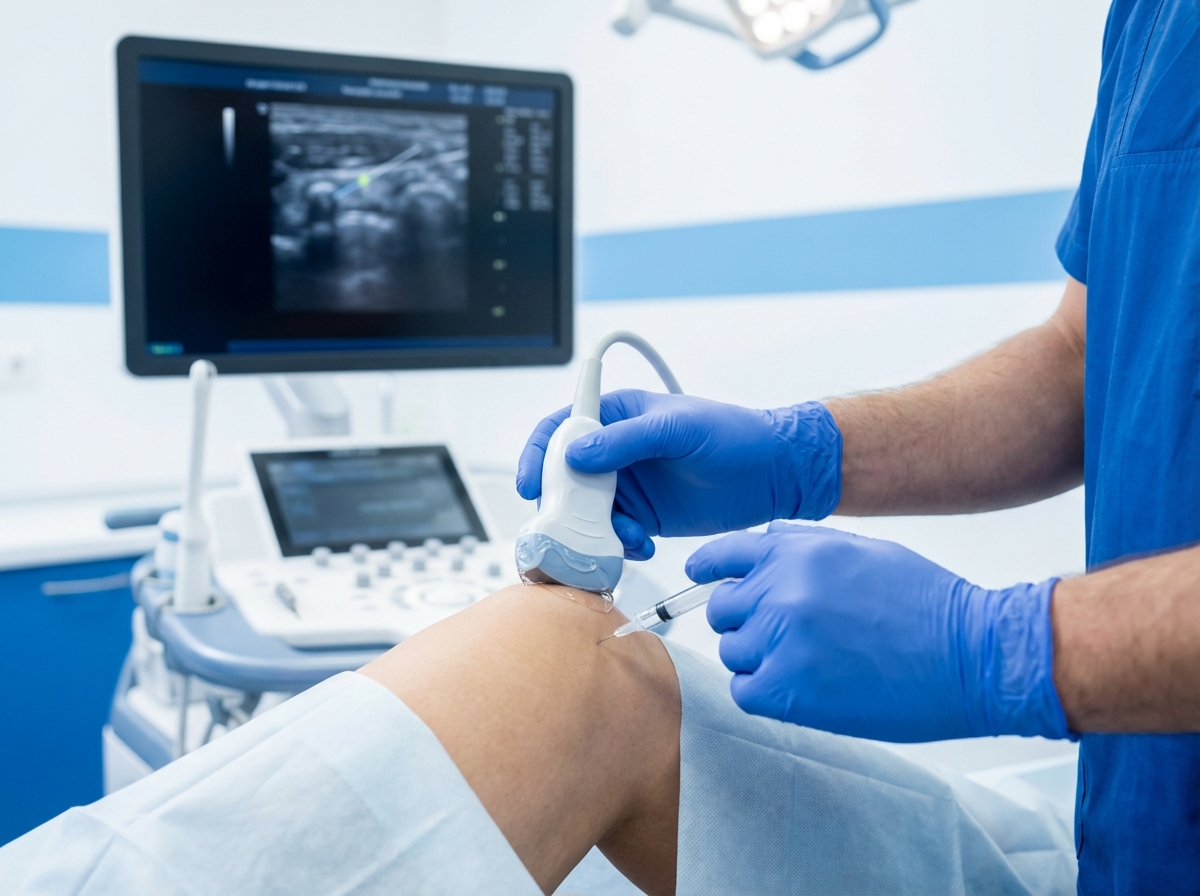
PRP Injection with Ultrasound Guidance: The 96% Accuracy Standard That Protects Your Investment
PRP Injection with Ultrasound Guidance: The 96% Accuracy Standard That Protects Your Investment
Platelet-rich plasma therapy represents a significant investment—both financial and biological. Patients commit their own concentrated platelets, their time, and their resources toward healing damaged tissue. Yet this investment faces a critical vulnerability that many patients never consider: PRP’s remarkable healing potential is completely wasted if platelet degranulation occurs outside the target tissue.
The difference between therapeutic success and wasted treatment often comes down to a single factor: injection accuracy. Research from Seoul demonstrates this clearly—ultrasound-guided knee injections achieve 96% accuracy compared to 83.7% with palpation alone. That 12% difference represents the margin between optimal outcomes and partial treatment failure.
Ultrasound guidance is not an optional upgrade or premium add-on. It represents essential due diligence that protects the patient’s investment in healing. Understanding why precision matters biologically, what the accuracy gap means economically, and how imaging guidance has become the standard of care empowers patients to make informed decisions about their treatment.
The Biology of Precision: Why PRP Placement Determines Treatment Success
PRP therapy works through a precise biological mechanism. Concentrated growth factors must reach the exact site of tissue damage to stimulate healing. These growth factors stimulate reparative cells and significantly enhance the natural healing process—but only when delivered to the precise location where tissue repair is needed.
When platelet degranulation occurs outside the target tissue, the consequences are significant. Healing potential diminishes, patient outcomes suffer, and the risk of adverse effects increases. The biological material that could have accelerated recovery instead disperses into surrounding tissue where it provides minimal therapeutic benefit.
PRP is fundamentally different from systemic treatments that circulate throughout the body. It functions as a localized therapy where millimeters matter. The concentrated platelets need direct contact with damaged tissue to release their growth factors effectively. Misplaced PRP means the patient’s own biological material—carefully extracted, processed, and concentrated—is essentially wasted.
The Accuracy Gap: Quantifying the Difference Between Blind and Guided Injections
The data on injection accuracy reveals a substantial gap between blind and guided techniques. Landmark-based injections range from 30-83.7% accuracy across multiple anatomical locations, while ultrasound guidance consistently achieves 90-100% accuracy.
The Seoul study’s findings on knee injections are particularly instructive: 96% accuracy with ultrasound guidance versus 83.7% with palpation alone, a difference that achieved statistical significance (p < 0.05). This 12% accuracy improvement represents real-world treatment outcomes for patients.
A December 2025 systematic review of glenohumeral joint injections found even more dramatic differences. Ultrasound-guided injections achieved 63-100% accuracy compared to just 40-76% with blind injection techniques. Landmark-based accuracies typically fall in the low to mid-60s across anatomical locations—meaning roughly one-third of blind injections miss their intended target.
The accuracy challenge intensifies in complex scenarios. Patients with severe osteoarthritis and joint deformity, those with obesity, or individuals with complex anatomy face even lower success rates with blind injection techniques. Without imaging guidance, blind knee injections achieve only approximately 70% accuracy—and this figure decreases further when anatomical challenges are present.
What the 12% Accuracy Difference Means for Treatment Investment
Framing the 96% versus 83.7% accuracy gap in economic terms reveals its true significance. This difference represents the margin between optimal return on investment and partial treatment failure.
If nearly 1 in 6 blind injections miss the target, patients may require repeat procedures or experience suboptimal outcomes. Cost-effectiveness data supports this concern: studies demonstrate a 58% reduction in cost-per-responder ratios when ultrasound guidance is employed.
The “dry knee” scenario presents particular challenges. In patients with advanced arthritis where synovial fluid is minimal, traditional aspiration confirmation methods fail. Imaging guidance becomes essential to verify proper needle placement when other confirmation methods are unavailable.
A 2025 network meta-analysis demonstrates PRP’s superior performance, ranking highest with SUCRA values of 85.86% for total WOMAC score, 78.55% for pain, 93.24% for stiffness, and 90.9% for function. However, these impressive outcomes depend entirely on proper delivery. Precision allows for greater effect with lower doses, maximizing the value of each treatment when the concentrated platelets reach their intended destination.
Beyond Accuracy: The Clinical Advantages of Real-Time Visualization
Real-time visualization transforms the injection procedure from a blind technique into a precision-guided treatment. Clinicians can assess tissue condition and tailor PRP treatment to specific patient needs during the procedure itself. This dynamic assessment capability allows for adjustments that optimize treatment delivery.
Safety advantages compound these benefits. The ability to visualize nerves and blood vessels in real-time reduces the risk of complications and tissue damage. Unlike fluoroscopy-guided injections, ultrasound involves no radiation exposure while maintaining superior soft tissue visualization.
Consistency represents another significant advantage. Research demonstrates that ultrasound guidance achieves 100% accuracy regardless of injector experience level, eliminating variability that can affect outcomes with blind techniques. Studies consistently show ultrasound-guided injections result in better patient satisfaction scores.
The Evidence Standard: Why PRP with Ultrasound Guidance Delivers Superior Outcomes
The evidence supporting ultrasound-guided PRP delivery continues to strengthen. The 2025 network meta-analysis found PRP ranked highest across multiple outcomes with SUCRA values of 85.86% for total WOMAC score, 78.55% for pain, 93.24% for stiffness, and 90.9% for function.
The regenerative medicine field continues advancing rapidly. Currently, 224 clinical trials globally are investigating stem cell therapies for osteoarthritis, with a major Phase III clinical trial funded with $140 million announced in January 2026. As these advanced therapies develop, precision delivery becomes increasingly critical.
Ultrasound-guided injections prove more accurate than landmark-guided techniques across all anatomic locations studied. Diagnostic imaging outcome assessments including ultrasound-guided needle precision are now standard components of research protocols, reflecting the scientific consensus on the importance of accurate delivery.
When Ultrasound Guidance Becomes Essential: Complex Cases and Challenging Anatomy
Certain patient populations face heightened risk from blind injection techniques. Patients with severe osteoarthritis and joint deformity present altered anatomy that makes landmark-based approaches unreliable. Obesity creates similar challenges by obscuring anatomical landmarks. Previous surgery with altered anatomy compounds these difficulties.
Difficult-to-access joints present particular challenges for blind techniques. Hip injections, small hand joints, and deep anatomical structures cannot be reliably accessed through palpation alone. The accuracy data for these complex anatomical locations strongly favors imaging guidance.
The “dry joint” scenario—patients with advanced arthritis where synovial fluid is minimal—eliminates traditional confirmation methods. Without the ability to aspirate fluid to verify needle placement, imaging guidance provides the only reliable confirmation of accurate delivery.
Ultrasound allows treatment of multiple sites in a single session while maintaining accuracy at each location. This capability proves valuable for patients with multiple areas of concern. As PRP therapy becomes more sophisticated with optimized concentrations and formulations, precision delivery becomes even more critical to achieving optimal outcomes.
The Unicorn Bioscience Standard: Imaging-Guided Precision as Default Practice
Unicorn Bioscience has established imaging-guided precision as standard practice across all locations. All injections are administered using advanced imaging guidance, including ultrasound and X-ray technology—not as an optional upgrade, but as the default approach to treatment.
This commitment to precision directly protects patients’ investment in PRP therapy. Imaging guidance ensures that both the financial and biological resources patients commit to treatment are protected through accurate delivery to target tissue.
The personalized treatment planning approach leverages ultrasound’s real-time assessment capabilities. Treatment protocols are developed based on individual patient factors including inflammation levels, age, injury type, and tissue condition observed during the procedure. This dynamic assessment allows for optimization that blind techniques cannot provide.
The multi-modal treatment capability—including PRP, BMAC, stem cells, exosomes, and hyaluronic acid—benefits from precision imaging across all treatment types. Accurate delivery matters regardless of the specific regenerative therapy being administered.
Consistency extends across all eight locations in Texas, Florida, and New York. Patients receive the same imaging-guided precision standard whether they visit Austin, Dallas, El Paso, Fort Worth, Houston, San Antonio, Boca Raton, or Manhattan. The medical team’s training at institutions including Johns Hopkins and Hospital for Special Surgery brings institutional precision standards to every procedure.
Making an Informed Decision: Questions to Ask Providers
Patients considering PRP therapy should ask specific questions to ensure they receive precision-guided treatment:
- “Do you use ultrasound guidance for all PRP injections or only in certain cases?” Standard practice should include imaging guidance for all procedures.
- “How do you confirm the injection reached the target tissue?” Real-time visualization provides immediate confirmation of accurate placement.
- “What is your documented accuracy rate with imaging-guided injections?” Providers should be able to discuss their outcomes data.
- “What imaging technology do you use and is it available at every appointment?” Equipment availability should be consistent, not dependent on scheduling.
- “How do you measure treatment success and what percentage of your patients achieve their therapeutic goals?” Outcome tracking demonstrates commitment to results.
- “What happens if the injection doesn’t reach the target tissue?” Understanding protocols for suboptimal placement reveals provider quality standards.
These questions help patients protect their investment by ensuring they receive precision-guided treatment from providers committed to accuracy.
Conclusion
PRP therapy represents a significant commitment of resources and biological material that deserves precision delivery. The 96% versus 83.7% accuracy difference is not merely a statistic—it represents the margin between therapeutic success and wasted treatment.
Ultrasound guidance has evolved from optional enhancement to essential standard of care based on overwhelming evidence. The 2025 network meta-analysis demonstrating PRP’s superiority applies only when treatment is accurately delivered to target tissue. Misplaced injections cannot deliver the outcomes that research demonstrates are achievable.
Patients who understand the accuracy gap can make informed decisions about their treatment providers. The economic reality is clear: protecting a PRP investment begins with ensuring precision-guided delivery from the first injection.
Experience the 96% Accuracy Standard at Unicorn Bioscience
Imaging-guided precision is standard practice at all eight Unicorn Bioscience locations—not an optional upgrade. Qualified candidates may receive same-day treatment with precision-guided injection technology.
Virtual and in-person consultations are available to discuss personalized treatment planning. Schedule a consultation to learn how ultrasound-guided PRP therapy can protect investment in healing.
Contact: (737) 347-0446
Locations: Austin, Dallas, El Paso, Fort Worth, Houston, San Antonio (Texas) | Boca Raton (Florida) | Manhattan (New York)
Don’t leave PRP therapy to chance—choose the precision that protects investment.
Schedule Your Consultation Today!