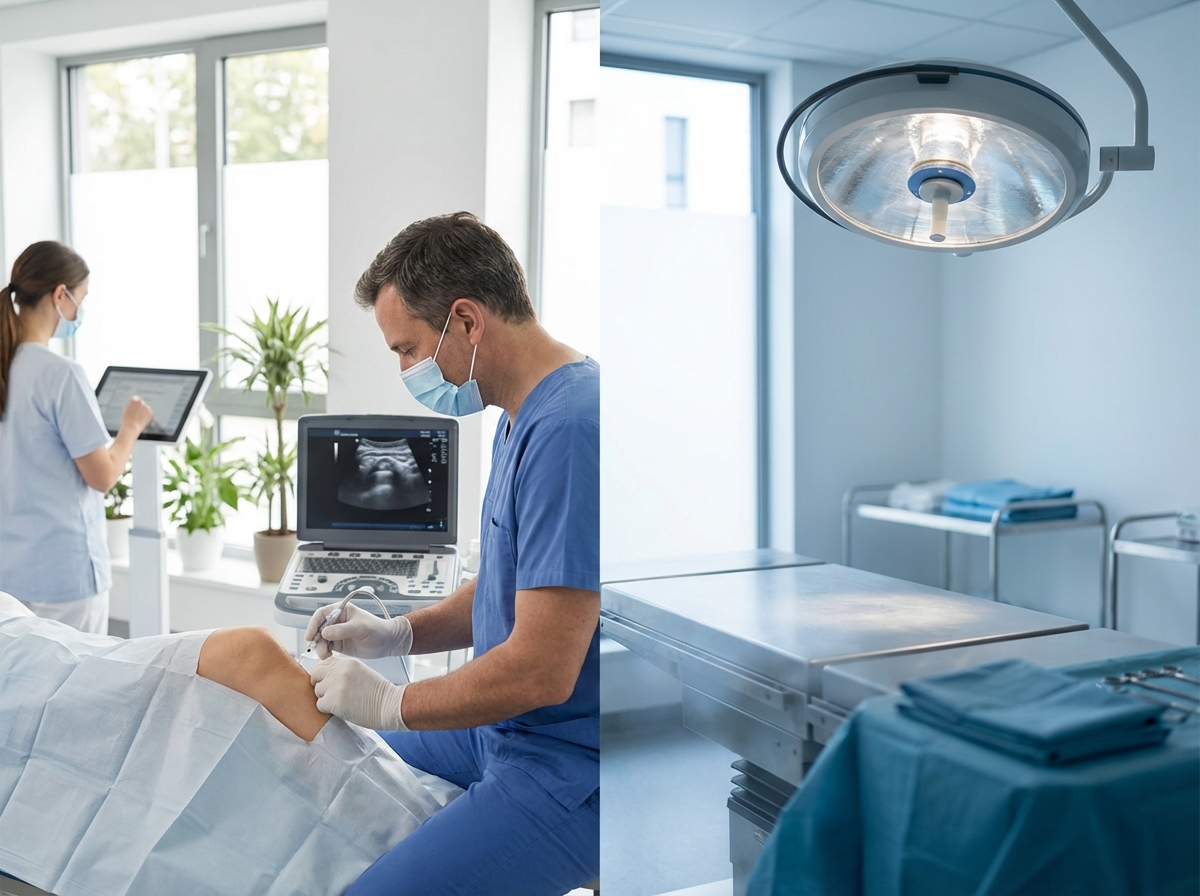
Stem Cell Injection Side Effects Risks: The 12.3% Temporary Reaction Rate vs. Surgery’s 2-10% Infection Reality
Stem Cell Injection Side Effects Risks: Temporary Reaction Rates vs. Surgery’s 2-10% Infection Reality
When patients face orthopedic injuries or degenerative conditions, the question of treatment safety often becomes paramount. Understanding actual risk data—rather than relying on assumptions or anecdotal information—empowers individuals to make truly informed healthcare decisions. This article presents a transparent, evidence-based comparison of stem cell injection side effects against surgical alternatives, using concrete numerical data from peer-reviewed clinical research.
The central framework for this comparison centers on temporary reaction rates for stem cell therapy versus infection rates for surgical interventions. A landmark 2021 meta-analysis examining 62 randomized trials with 3,546 participants found zero serious adverse events associated with mesenchymal stem cell treatments—no deaths, infections, sepsis, neoplasms, or embolisms. This data provides a foundation for patients seeking quantifiable risk assessments rather than vague reassurances about “lower risk” treatments.
The Evidence-Based Safety Profile: What Clinical Data Actually Shows
The most comprehensive safety data available comes from systematic reviews and meta-analyses that aggregate outcomes across multiple clinical trials. The 2021 meta-analysis published in peer-reviewed medical literature examined 62 randomized clinical trials encompassing 3,546 participants. The findings were striking: researchers discovered no serious adverse events such as death or infection across all included studies.
The most commonly reported side effect category represents transient swelling and pain at the injection site lasting less than four weeks. This reaction is self-limiting and typically requires no medical intervention. Transient fever occurs in approximately 22% of cases depending on the condition being treated, representing the most frequent systemic response to mesenchymal stem cell therapy.
Long-term safety monitoring extending to five-year follow-up periods has demonstrated sustained safety profiles without delayed complications. As of early 2025, over 1,200 patients have been dosed with pluripotent stem cell products—more than 10^11 cells administered—with no generalizable safety concerns reported across ophthalmology, neurology, and oncology applications.
Minor vs. Serious Adverse Events: Understanding the Risk Categories
Distinguishing between minor and serious adverse events is essential for accurate risk assessment. Minor or transient adverse events include temporary discomfort, localized swelling at the injection site, and brief fever episodes that resolve without medical intervention. These reactions represent the body’s natural response to the therapeutic procedure and typically dissipate within days to weeks.
Serious adverse events encompass infection, sepsis, tumor formation, embolism, death, and permanent complications requiring additional medical treatment or hospitalization. The critical finding from systematic reviews of autologous mesenchymal stem cell injections is the absence of these major complications in properly conducted treatments.
This distinction matters significantly when comparing treatment options. While some stem cell patients may experience temporary injection site reactions, zero percent in comprehensive meta-analyses experienced complications requiring hospitalization or additional medical intervention. Surgical complications, by contrast, frequently necessitate extended hospital stays, antibiotic treatments, or revision procedures.
The Risk Assessment Matrix: 100 Stem Cell Patients vs. 100 Surgical Patients
To make risk comparison tangible, consider what happens to 100 patients in each treatment group based on clinical evidence:
Stem Cell Therapy Group (100 patients):
- Some patients experience temporary injection site reactions (swelling, mild pain)
- Approximately 22 patients may experience brief fever lasting 24-48 hours
- 0 patients develop serious infections
- 0 patients experience blood clots or embolism
- 0 deaths
- Recovery timeline: Days to return to normal activities
Surgical Group (100 patients):
- 2-10 patients develop surgical site infections
- Additional patients face blood clot risks (deep vein thrombosis, pulmonary embolism)
- Anesthesia-related complications affect a subset of patients
- Recovery timeline: 4-6 months for full rehabilitation
- Extended hospitalization required
The invasiveness differential is substantial. Stem cell procedures involve no large incisions, no general anesthesia, and no hospitalization. Recovery time is reduced by more than 60% compared to surgical alternatives—a factor that significantly impacts quality of life and return to normal activities.
Surgical Risk Reality: The 2-10% Infection Rate and Beyond
Surgical interventions carry a cumulative risk profile that extends beyond the headline infection rate. The 2-10% infection rate varies based on procedure type, patient health factors, and surgical environment. However, infection represents only one category of surgical risk.
Anesthesia-related complications include cardiovascular events, respiratory issues, and adverse drug reactions. While modern anesthesia is generally safe, these risks are eliminated entirely with stem cell injections that require only local anesthesia.
Blood clot risks following orthopedic surgery include deep vein thrombosis and pulmonary embolism—potentially life-threatening complications that require anticoagulant therapy and ongoing monitoring.
Extended recovery complications encompass muscle atrophy during immobilization, joint stiffness requiring intensive physical therapy, and rehabilitation challenges that can persist for months. The 4-6 month recovery period for major orthopedic surgeries represents a significant quality-of-life impact that compounds other risk factors.
Why Autologous Mesenchymal Stem Cells Have Superior Safety Profiles
The exceptional safety record of mesenchymal stem cell therapy stems from several biological and procedural factors. Autologous treatments—using the patient’s own cells—eliminate immune rejection risks and disease transmission concerns entirely. The body recognizes its own cellular material, preventing the inflammatory responses that can occur with foreign tissue.
Mesenchymal stem cells possess inherent immunomodulatory properties and low immunogenicity, meaning they naturally avoid triggering immune system attacks. This characteristic contributes to both their therapeutic effects and their safety profile.
Regarding tumor formation concerns, MSCs have demonstrated differentiation limitations and biological constraints that prevent uncontrolled growth. Long-term monitoring across multiple studies has confirmed the absence of tumor formation despite theoretical concerns raised during early research phases.
Wharton’s jelly MSCs and bone marrow-derived cells show superior safety profiles compared to embryonic or certain allogeneic sources, making source selection an important factor in treatment planning.
The Critical Role of Quality Control and Safety Protocols
The safety statistics cited throughout this article reflect outcomes from properly conducted treatments following established protocols. Good Manufacturing Practice (GMP) compliance forms the essential foundation for safe stem cell therapy, ensuring consistent quality and sterility throughout the preparation process.
Proper donor screening protocols include infectious disease testing, comprehensive medical history evaluation, and quality assessments that identify any potential safety concerns before treatment proceeds. Sterile processing requirements encompass contamination prevention, controlled environments, and validated procedures that minimize procedural risks.
Advanced imaging guidance represents a significant safety enhancement in modern stem cell therapy. Precision-guided injection protocols using ultrasound and X-ray technology ensure accurate delivery of therapeutic cells to targeted treatment areas. Unicorn Bioscience employs these imaging technologies across all injection procedures, reducing injection site reactions and enhancing therapeutic targeting.
Unicorn’s Safety Standards: Minimizing Even Minor Side Effects
Unicorn Bioscience has implemented comprehensive safety measures designed to minimize even the minor, transient side effects associated with stem cell therapy. The practice maintains GMP-compliant safety standards and quality control measures throughout the treatment process.
The precision-guided injection technology—utilizing both ultrasound and X-ray guidance—reduces injection site reactions by ensuring accurate needle placement and optimal cell delivery. This technology represents a technical advantage that directly impacts patient comfort and outcomes.
Personalized treatment planning considers multiple individual factors: inflammation levels, patient age, injury type and location, current medications, and personal health goals. This comprehensive assessment allows providers to select the optimal treatment modality from available options including PRP, BMAC, exosomes, and stem cell preparations based on each patient’s specific risk-benefit profile.
Same-day treatment availability for qualified candidates follows comprehensive safety screening, ensuring that patients receive timely care without compromising safety protocols.
The Unregulated Clinic Danger: Why Facility Selection Matters
The FDA and NIH have issued explicit warnings about unregulated “stem cell tourism” clinics that operate outside established safety frameworks. The Pew Charitable Trusts gathered 360 reports of adverse events related to unapproved stem cell therapies between 2004 and 2020, including 20 cases that resulted in death. Documented adverse events from unregulated providers include infections, blindness, spinal tumors, and other serious complications.
The regulatory landscape is important to understand: currently, the only stem cell products that are FDA-approved for use in the United States consist of blood-forming stem cells derived from umbilical cord blood for specific blood disorders. Most orthopedic and regenerative applications remain investigational, though substantial clinical evidence supports their safety when administered by qualified providers within FDA regulatory frameworks.
Criteria for identifying legitimate providers include:
- Board-certified physicians with relevant training
- GMP-compliant facilities and protocols
- Transparent safety data and outcome tracking
- U.S.-based treatment within regulatory frameworks
- Advanced imaging guidance for injection procedures
Condition-Specific Safety Data: Knee Osteoarthritis and Beyond
Knee osteoarthritis represents one of the most extensively studied applications for stem cell therapy. Systematic reviews examining autologous MSC injections for knee osteoarthritis have found no major complications, with treatment posing moderate risk only of swelling and pain at the injection site lasting less than four weeks.
Unicorn Bioscience reports that more than 90% of their stem cell patients have not gone on to knee replacement surgery, suggesting strong outcomes that may help patients avoid the higher-risk surgical alternative.
Safety profiles for other orthopedic conditions—including rotator cuff injuries, meniscus tears, and spine conditions—show similarly favorable data, though injection site and tissue type can influence specific risk profiles.
The field continues to advance rapidly. A major Phase III clinical trial funded with $140 million was announced in January 2026 by MEDIPOST for knee osteoarthritis treatment, reflecting continued investment in establishing the evidence base for these treatments.
Long-Term Safety Monitoring: What 5-Year Follow-Up Studies Reveal
Long-term safety data provides reassurance beyond immediate post-procedure outcomes. Five-year follow-up studies have demonstrated sustained safety without delayed complications, addressing concerns about potential long-term adverse effects.
The absence of tumor formation in long-term monitoring is particularly significant given early theoretical concerns about stem cell proliferation. Ongoing surveillance requirements and post-treatment monitoring protocols continue to generate safety data as the field matures.
The 2025 MDPI biosafety framework proposes operational principles for assessing stem cell therapy safety across five key domains: toxicity, oncogenicity, immunogenicity, biodistribution, and cell product quality. This framework reflects the field’s commitment to rigorous safety evaluation as treatments become more widely available.
Making an Informed Decision: Risk-Benefit Analysis Framework
Patients considering treatment options should weigh the temporary reaction rates of stem cell therapy against the 2-10% surgical infection rate plus additional surgical risks including anesthesia complications, blood clots, and extended recovery periods.
Recovery time comparison—days versus 4-6 months—represents a substantial quality-of-life factor that may influence treatment decisions for patients with work obligations, family responsibilities, or active lifestyles.
Individual risk factors including age, overall health, condition severity, and previous surgeries may influence optimal treatment selection. Surgery may remain appropriate for cases involving advanced degeneration or structural damage requiring reconstruction.
Consultation with qualified providers enables personalized risk assessment based on individual circumstances. Unicorn Bioscience offers both virtual and in-person consultations across eight locations in Texas, Florida, and New York.
Conclusion
The evidence-based safety profile of stem cell therapy presents a compelling case for patients seeking alternatives to knee replacement surgery and other surgical interventions. Zero serious adverse events in a meta-analysis of 3,546 patients stands in stark contrast to the measurable infection rates, blood clot risks, and anesthesia complications associated with orthopedic surgery.
The risk assessment demonstrates that while some stem cell patients experience temporary, self-limiting reactions, the absence of serious complications represents a fundamentally different risk category than surgical alternatives.
Facility selection remains critical—GMP compliance, precision-guided protocols, and qualified providers minimize even minor side effects while ensuring treatment quality. While orthopedic applications remain investigational under current FDA frameworks, substantial clinical evidence supports the safety of properly administered stem cell therapy.
Patients now have access to concrete clinical data enabling informed healthcare decisions based on actual outcomes rather than assumptions. For those seeking to explore whether stem cell therapy’s favorable safety profile makes it appropriate for their specific condition, Unicorn Bioscience offers consultations at locations across Texas, Florida, and New York. Contact (737) 347-0446 or visit unicornbioscience.com to begin the evaluation process.
Schedule Your Consultation Today!